National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
3 min read
 Brittany Means, RN, BSN
:
Jan 22, 2021
Brittany Means, RN, BSN
:
Jan 22, 2021

Picture this:
About 12 hours into your 24-hour shift, you and your partner are finally sitting down to your first real meal of the day.
Just as the first bite of warm food hits your lips, the tones drop—an all-too-familiar scenario in the world of first responders.
You’re dispatched to a 51-year-old male reporting chest pain. You walk in the door to a very distraught family, gathered around a man clutching his chest. He is pale and sweating profusely. You meet your partner’s eyes, and you know you’re both thinking the same thing. You quickly obtain the ECG and your suspicions are confirmed: tombstones in leads II, III, and AVF.
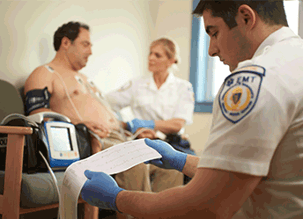 To you and your partner, this isn’t just a STEMI. This is a father, grandfather, and best friend to the wide-eyed and fearful family you leave behind as you expedite him to the nearest PCI facility.
To you and your partner, this isn’t just a STEMI. This is a father, grandfather, and best friend to the wide-eyed and fearful family you leave behind as you expedite him to the nearest PCI facility.
Caring for patients experiencing time-sensitive emergencies is much like running a 400-meter relay. It doesn’t matter how quickly leg 1 and leg 2 run the race if leg 3 is bent over tying his shoelaces, not ready to receive the baton when leg 2 hands it to him. How effective is this spectacular pre-hospital performance if, upon arrival, the ER and receiving care teams are not yet ready to treat this patient?
The glory of an 8-minute scene time is tainted when the patient is left to wait in the emergency room for 15 minutes while the care team continues to arrive and prepare for treatment. While the ER quickly jumps in to administer Aspirin and Nitro, everyone feels the same sense of helpless urgency, as this man’s only hope lies in the Cath Lab.
That's why it's crucial to mobilize the entire care team early in time-sensitive situations. EMS and hospitals have tried many solutions to bring the whole care team on board as quickly as possible: pre-hospital ECG transmission to the ED, paging and text alert systems, overhead announcements, games of phone tag between the operator and care team… the list goes on and on. The problem with these types of approaches is the variability across protocols. Each team has their own way to communicate, and most of these methods only go from point-to-point. This means you're playing a long game of telephone to get the right information to the right people at the right time—increasing the chance for error and the amount of precious time wasted.
 Your challenge: How do you effectively and consistently mobilize your receiving care teams? Are you sprinting out of the gate, only to fall behind halfway through the race?
Your challenge: How do you effectively and consistently mobilize your receiving care teams? Are you sprinting out of the gate, only to fall behind halfway through the race?
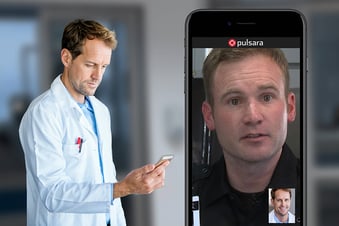
This is 2026. Our smartphones are capable of turning off all the lights in our house and remotely closing the garage door. Wouldn’t it be great if we could utilize this tool that we all have in our back pockets for... COMMUNICATION?
Pulsara can help you streamline communication and care coordination by enabling you to mobilize receiving care teams within seconds, ultimately saving precious minutes. When time is tissue, every second counts!
CHRISTUS Good Shepherd Medical Center - Longview in Longview, Texas struggled with synchronizing their stroke team on one universal clock. In an effort to make sure all members of the care team were watching the same clock, CHRISTUS Good Shepherd implemented Pulsara. In 2020, they reported a 46-minute average door-to-needle for patients receiving tPA, a 59% decrease from their previous average time of 110 minutes. They now have 100% of their door-to-needle completed in under 60 minutes—and 58% in under 30 minutes.
In 2020, Latrobe Regional Hospital near Melbourne, Australia, used Pulsara to streamline communication between their ED staff and Ambulance Victoria. Within a year, they reduced their already excellent door-to-CT times for stroke by 68%.
After implementing Pulsara to efficiently transmit ECGs between EMS and their hospital teams and improve communications, Saline Memorial Hospital in Saline County, Arkansas, reduced first medical contact-to-device times by 28% over four months, a full 15-minutes under the ACC and AHA recommendations.
By improving communication and fostering a greater awareness of the passage of time between the members of their stroke team, these facilities have significantly increased their patients' chances for positive outcomes.
How can Pulsara help transform your STEMI care and your bottom line? Learn more here.
Editor's Note: This post was originally published in March of 2015 and has been refreshed and updated for accuracy and comprehensiveness.
To learn more about how hospitals and EMS organizations are using Pulsara to improve communication, reduce treatment times, and mitigate the spread of COVID-19, check out more of our customer success stories.

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...