National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
9 min read
 Team Pulsara
:
Dec 01, 2021
Team Pulsara
:
Dec 01, 2021

The past two years have done a great deal to redefine the shifting identity of EMS. COVID-19 changed a lot about how we provide care, and some of the solutions we came up with have led to a watershed of self-discovery. With that, though, comes an equal number of questions. What does the shifting landscape of healthcare mean for EMS? What will the role of EMS be going forward? As the identity of EMS evolves and medics are given more agency, will they be able to help find solutions for problems like overcrowded emergency departments, while also giving patients both a better and more appropriate care experience?
Corey Ricketson, Pulsara's Vice President of Strategic Accounts, recently had the opportunity to discuss these and other hot topics in EMS with Chris Cebollero on The Inside EMS podcast, hosted by EMS1. Corey shares his experiences visiting multiple EMS agencies throughout the country, as well as some top takeaways from how leading EMS agencies are finding solutions to issues like ED overcrowding. Chris and Corey talk community paramedicine, how EMS needs to adapt for the future, the importance of meeting patients where they are, and how interoperability, connection, and communication should be a main focus for EMS agencies.
Listen to the podcast below, and read on for part 2 of the interview! (If you missed part 1, check it out here.)
NOTE: This transcript has been edited for brevity and clarity.
Chris Cebollero:
All right. We're back with Corey Ricketson, [Vice President of Strategic Accounts] at Pulsara. So, we kind of set it up right before we went to the break. We talked about emergency management. One of the things that I think that we're not great at is preparing ourselves for the timeframe when we have to be able to [expand our response] in emergency management. Let's kind of touch on that a little bit. So from your side, have you noticed any trends in emergency management that are really something that we've got to address, or something that we've got to look at, or something we've got to prepare for?
Corey Ricketson:
Absolutely, yeah. I mean, I think that this pandemic has certainly highlighted the gaps that we have in the healthcare system as a whole. One of the things that I see daily is—I'm going to call it the supply side and the demand side. So on the supply side, you have a lot of hospitals that have to report their bed capacity, because of federal regulations or local regional regulations. Right? Well, those numbers are never right. They're just not. As much as they try, the supply side is off. And so at that point, you have, maybe it's a rural hospital that says, "I need to transfer a patient." And I'm looking at this capacity management and I see that your health system is saying that you have five ICU beds available. Yet, when I call your transfer center, there are no beds available, and the data was flawed.
And then you have a lot of states and regions that are completely in the dark on the demand side as well. How many patients need to get transferred or moved? What is the best way to communicate about that? Because now, a lot of these patients are not staying within their local areas. I mean, we've got patients being moved across state lines—and not just the next state over, 10 states over—in order to be able to find a bed. So that movement is not a small feat, and it takes all of us kind of rolling our sleeves up and being interconnected in order to solve that problem.
So let me bring up an example. When I was deployed out to El Paso when they had their big surge, in the first 48 hours when I got there, there were airplanes coming in to get patients. They were getting the wrong patient, potentially. They were taking off, and the patient has an adverse event, and they need to come back and land and take them back to the sending facility because of stability. You can imagine how many phone calls it takes in order to orchestrate the event in the first place. You've got a sending hospital. You've got a local or regional coordination center. You've got transfer centers and receiving hospitals and receiving docs and sending docs. Those are all phone calls.

And so when that patient has that adverse event and they have to come back to that first facility, how many phone calls do you think it takes in order to keep everyone with situational awareness abreast of what's going on? Thirty-plus phone calls is what we calculated. Once we deployed the solution and we literally had sending hospitals, statewide coordination centers, regional coordination centers, MOCCs. You might hear the FEMA term of medical operation coordination cells. When all of those people are on the same communications platform, then literally it's like sending a group text and saying, "Patient's crashing, returning to first facility." Guess who knows immediately? Every single person that needed to know and that has some type of a stake in that patient's care is immediately kept up to speed.
So in the emergency management realm, we have a lot of solutions that sat on shelves. I mean, I was deployed to Hurricane Katrina. And as a triage officer, how many triage tags do you think I used? Zero. Because it wasn't familiar. And we have a lot of things that we purchase that we're expected to use on the worst day of our life—but it's not familiar to us... So, one of the things that we're seeing as a trend is this concept of systems of care that scale. Use the same thing daily. So in my everyday EMS transmission to the hospital, I'm going to use this communications platform. We're going to build muscle memory, and that's what we're going to use, to get familiar with it.
And when a patient needs to get transferred, we're going to use that same thing, to build that muscle memory. That way, when we do have a stress event, every day's disaster day. It's business as normal. There's really no change; it just breathes in and breathes out. It scales to an EOC in a crisis. And then it scales back down when the stress event's gone.
Chris Cebollero:
One of the things that you brought up that I didn't really consider in this whole practice of COVID was, in the event of an MCI, or in the event of a mass shooting, or in the event of anything that's going to be a multi-casualty, there may not be any place for them to go, because all these hospitals are just crazy with their census. We hear all the time that there are no beds. And you bring up the great point that we may have to send these people out of state. We may have to fly these people. And certainly, we've got to worry about trauma patients. But we may be sending them within the same state, miles and miles away because our local level-one trauma center doesn't have the ability to take care of them.
Corey Ricketson:
Right. No, it's absolutely what's happening. And you hear of it all over the place, where even for something that's not major, the patient can't get the right treatment. I was just on a call last night trying to help find placement for a patient. And actually, one of the places that I think we may have found was in St. Louis. And this patient's sitting in Texas. So it's the different world that we're living in. Interoperability could not be more important right now. And clearly, what we have sitting on the shelf nationwide is not working. And so there's got to be a different methodology to tackle the problem.

Chris Cebollero:
I think that's a great way to put it. So let me ask you this question. You talked about interoperability. When we think about connectivity—and it's a shame that 20 years after 9/11, we're still having connectivity and interoperability challenges. When we think about the benefit of uniting the care team and being able to discuss things across multiple organizations or multiple platforms, what are the secrets to ensuring that we can make this happen, and do it in a way that is really taking care of the sick guy [and ensuring we have the resources to properly take care of the patient]?
Corey Ricketson:
Yes. You think about the way healthcare's decentralized now. And being able to connect the right people that have a stake in that patient's care, regardless of whether they're in the same physical brick-and-mortar facility, is of the utmost importance. Say you have a patient that's sitting in a rural hospital, and number one, we've got to find a place for them. Number two, once we do find a place for them, we've got to keep everyone abreast of the situation and up to speed. What's this patient's ETA going to be? Has EMS even gone and picked them up, or the helicopter, or the airplane? And what is their status?
Those people, those stakeholders, are in multiple different places. They're in transfer centers. They're at sending hospitals. They're at receiving hospitals. They have private practices. I'm a pulmonologist. I'm a hospitalist. Every one of those people needs to be connected. And if you think about how we do business, Chris—if we wanted to coordinate a dinner tonight with five of our friends, we would start a group chat. I mean, it's just what we do. It's everyday life and it's so familiar. Yet, when we get in a healthcare situation, that completely breaks down and we're back to fax, phone, radio. And we're like, "Where are we right now? Why can't we just ..." I mean, [in the way we now communicate as a society], if I wanted to get a cardiologist and a cath lab together, and if HIPAA weren't a concern, I would walk in and probably take a selfie with the 12 lead and say, hashtag widowmaker, hashtag cardiology. And guess who would know immediately? All the people that need to know immediately. But we can't do that because of HIPAA.
That's where Pulsara comes in, quite honestly. We give you all the tools that you enjoy in everyday life communication, but in a healthcare-compliant platform, so that we can connect all of those people across organizations and allow them to collaborate. And they can do things like upload an image of this patient's lab values, so the pulmonologist, who's 1000 miles away, can see those.
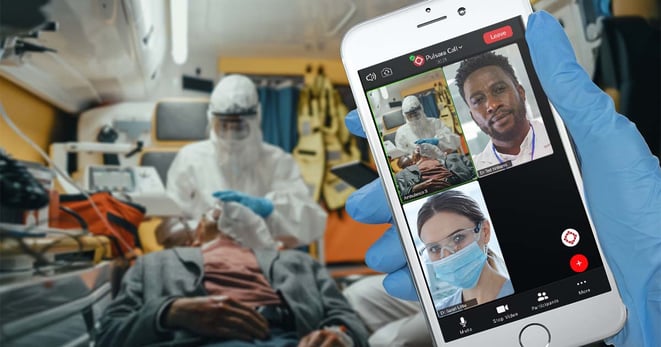
Or, I'm going to start a live video group call between five clinicians, and we're going to all converge on this patient, and we're going to take care of them. One of the things we've seen in Texas right now is that if we cannot move a patient, how can we bring the medicine to them? How can we bring specialists to a rural hospital and help that doctor or nurse with things like vent settings, or looking at lab values and trying to discern what the best mode of treatment is? And so it's thinking about this differently. The only way you can bring that type of medicine to a patient is to connect those care team members.
Chris Cebollero:
I think you hit a couple of great points there. And I think that it makes our job a little bit easier, too, when we think about this from the transportation officer side; when we've got to be able to figure out resources, or we've got to be able to connect people. I think it makes our job easier. So one of the big things, Corey, in EMS certainly, is situational awareness. We've got to make sure that we have our hands on everything that's going on around us. And we've got to be able to bring as many people as we can into this process. It's not only healthcare providers that need to be given information when it's time for them to share, but there may be people outside EMS, outside of the healthcare realm, that need to be kept in the loop as well. So when we think about that from a situation awareness standpoint, how do we address that?
Corey Ricketson:
That's a good point. I mean, a lot of us have heard the terminology of RACI: Responsible, Accountable, Consulted, and Informed. And in every situation, there are people that have those roles. Right? It's why carbon copy came to be in emails because I need somebody else to be informed about this, but that's not necessarily who I'm directly talking to.

So think about a situation where maybe you're giving blood products in the field. You may need one of your supervisors to be informed about that. You may need the blood bank to be informed about that. So it's almost a way to bring the right people into the situation and share potentially sensitive information that you can't do over email. But in the heat of the moment, you can simply bring those parties into the channel for collaboration. They may not actually enter the group chat and give any information, but they're informed or consulted so that they have that situational awareness. That way, we are holistically treating this patient, and all of the different parties are aware of what's going on.
Chris Cebollero:
I've got to tell you, Corey, we've had a great time visiting today. And certainly, I've learned a lot, and hopefully the people out there are getting value out of your expertise. If you want to give people a final thought, what do you leave them with?
Corey Ricketson:
It's about connecting teams. I really think that in the future of EMS, we have a huge opportunity to rise to the occasion and actually be a hero in this situation and reduce surge, and actually do business in a more responsible manner. But you have to have a way to communicate and bring in people across organizations in order to succeed.
Chris Cebollero:
Very good. I want to thank you for joining us on the Inside EMS Podcast. And Corey Ricketson, Vice President of Strategic Accounts for Pulsara, it was great to have you on the show. Promise you're going to come back again and share some great information with us and the listeners.
Corey Ricketson:
Yeah. Great talking to you, Chris, I appreciate it.
Chris Cebollero:
And for everybody out there, I want to thank you for joining us on the Inside EMS Podcast. And you kind of heard what we think. We want to hear what you think. Go ahead and send us an email at the show at EMS1.com and allow us to know what you're thinking, and maybe you've got some ideas for some future shows, you want to be able to join us as well. For Kelly Grayson, I'm Chris Cebollero, and we look forward to seeing you guys again next week.
With a scalable system of care, Austin-Travis County EMS kept 434 low-acuity patients out of the hospital over just three weeks—and rerouted them to faster, more appropriate care. Here's how they did it.

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...