National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
4 min read
 Team Pulsara
:
Nov 13, 2020
Team Pulsara
:
Nov 13, 2020

EDITOR'S NOTE: Special thanks to Greg Brown, MN, RN, for writing today's blog post. You can connect with him on LinkedIn.
If you’ve ever done long shift work in the hospital setting, you know how taxing it can be. Being on for a long stretch is both mentally and physically exhausting. When that work falls on off-hours, those stressors are magnified. Working nights and weekends adds an immense layer of complexity to already high-risk situations. Emergencies don’t slow down after hours. STEMIs, traumas, and codes all arrive during the night, just the same as during the day, but with less staff present and fewer resources, you also have to deal with calling in all the necessary members of the care team.
My entire bedside career was done during off-hours—that night shift differential really adds up, after all. I always took pride in the fact that my team and I were high-performing clinicians. Despite not having all service lines available on-site during night shift, my ED ran like a top. We prided ourselves on getting the job done in spite of the fact that we had less resources on campus.

A majority of services have only call teams available during off-hours. Wrangling call teams can involve a seemingly endless number of variables...and these variables inevitably lead to delays in care for patients. Coordinating care with off-site clinicians in the middle of the night can lead to some pretty ineffective communication.
Whenever I had to alert a specialty care team, it was usually done via our health unit coordinator (HUC). I would pop my head out of the curtain and ask for the team to be activated. This would set into motion a chain of events that was seemingly endless—and inefficient. Phone calls would be made, and pages would be sent out into the abyss. Point-to-point communication meant that the ED clinicians worked in an almost completely siloed environment while the care coordination was happening. During times of ambiguity, our only option was to “page them again.” We were flying blind until we got word that the care team had arrived, or until they just showed up in the ED.
Many times, I watched this process lead to delays in patient care. I always chalked that up to being an unavoidable complication of off-hours care—the nature of the beast. I’d go through mental gymnastics trying to minimize the impact of those delays. But deep down, I always knew that those delays were not just minutes ticking away on a clock. Those minutes are tissue. Precious cells lost to the creeping invasion of ischemia. The more that are lost, the worse the outcome for the patient. Every minute of delay until they get treatment makes a difference to their quality of life once they recover.
 Unfortunately, clinical data verified my nursing instincts. According to Cardiovascular Business, “STEMI patients presenting during off-hours were not as likely as patients presenting during regular hours to undergo PCI within 90 minutes. Door-to-balloon times were 14.8 minutes longer as well.” This problem isn’t just limited to the United States. In a study of over 245,000 off-hours emergency admits in a large teaching hospital in England, there was an increased risk of mortality compared to those admitted during regular hours. Even worse, the mortality effect was additive; weekend nights were associated with the highest risk of mortality. Both studies found that many factors led into this difference in care, such as sleep deprivation and travel time for specialty teams. Those factors are difficult to mitigate.
Unfortunately, clinical data verified my nursing instincts. According to Cardiovascular Business, “STEMI patients presenting during off-hours were not as likely as patients presenting during regular hours to undergo PCI within 90 minutes. Door-to-balloon times were 14.8 minutes longer as well.” This problem isn’t just limited to the United States. In a study of over 245,000 off-hours emergency admits in a large teaching hospital in England, there was an increased risk of mortality compared to those admitted during regular hours. Even worse, the mortality effect was additive; weekend nights were associated with the highest risk of mortality. Both studies found that many factors led into this difference in care, such as sleep deprivation and travel time for specialty teams. Those factors are difficult to mitigate.
There is something we can fix, though: the archaic communication methods we use to coordinate our teams.
We already know that time is tissue, and that time-sensitive emergencies require a streamlined approach to care. It has also been well established that ineffective communication has a negative impact on care times for patients. Sub-optimal communication methods, compounded with off-hours risks and call team coordination, can lead to major delays in care for patients. Luckily, there is an easier way, and we can communicate like it's 2020, not 1982.
This is where, in my experience, using mobile technology for communication can save valuable time and cut down on delays in off-hours care. Connecting everyone in your care teams on one platform makes communication so much easier. What if you could alert all the people you needed with a few taps? Or reach your entire team with just one message? What if you could upload photos of the patient, or of their vital information, and share them with your entire team?
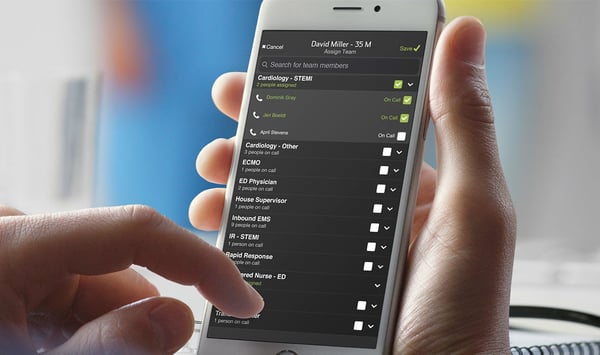
Pulsara offers an off-the-shelf, clinically proven way to streamline communication. With Pulsara, you can activate the care team with the touch of a button, send group messages to everyone on the team, upload photos, and even live video conference with other team members. Pulsara creates a dedicated channel for each patient, giving everyone throughout the entire multidisciplinary care team a shared consciousness about that patient. One-touch activation puts the entire team on the case, and communication can be done with a simple tap.
Think of the possibilities. Say the cath lab RN’s car won’t start, and it is 2 am. They would no longer need to call the operator and start making calls to the backup team. That cath lab RN can text the group and alert their replacement within seconds. THAT…is the power of streamlined communication! A problem that could cause minutes-long delays can be solved in a matter of seconds.
 The power of streamlined communication is evident in the success that organizations have had in driving down their care times after implementing Pulsara. On average, hospitals who use Pulsara see a 30% decrease in their time-to-treatment for STEMI and stroke. In a matter of months, Latrobe Regional Hospital near Melbourne, Australia, reduced their door-to-CT times from 22 minutes down to an average of just 7 minutes—a 68% reduction in treatment time.
The power of streamlined communication is evident in the success that organizations have had in driving down their care times after implementing Pulsara. On average, hospitals who use Pulsara see a 30% decrease in their time-to-treatment for STEMI and stroke. In a matter of months, Latrobe Regional Hospital near Melbourne, Australia, reduced their door-to-CT times from 22 minutes down to an average of just 7 minutes—a 68% reduction in treatment time.
After implementing Pulsara, CHRISTUS Good Shepherd Medical Center in Longview, Texas decreased their door-to-needle times by 59%, reporting a 46-minute average for patients receiving tPA, down from their previous average time of 110 minutes. They now have 100% of their door-to-needle completed in under 60 minutes.
In order to close the gap between outcomes for off-hours and normal hours, we need to remove every roadblock to rapid care—and that starts with simplifying our communication processes. When every member of the care team is united on one platform, we can get the right information to the right people at the right time. That means we can be there for patients when it matters most...especially during nights and weekends.
To learn more about how hospitals and EMS organizations are using Pulsara to improve communication, reduce treatment times, and manage large-scale pre-planned events, check out more of our customer success stories.

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...