National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
4 min read
 Team Pulsara
:
May 08, 2020
Team Pulsara
:
May 08, 2020
EDITOR'S NOTE: Special thanks to Kinsie Clarkson (Pulsara's Product Marketing Specialist, 2020-2025) for writing today's blog post. You can connect with her on LinkedIn.
__
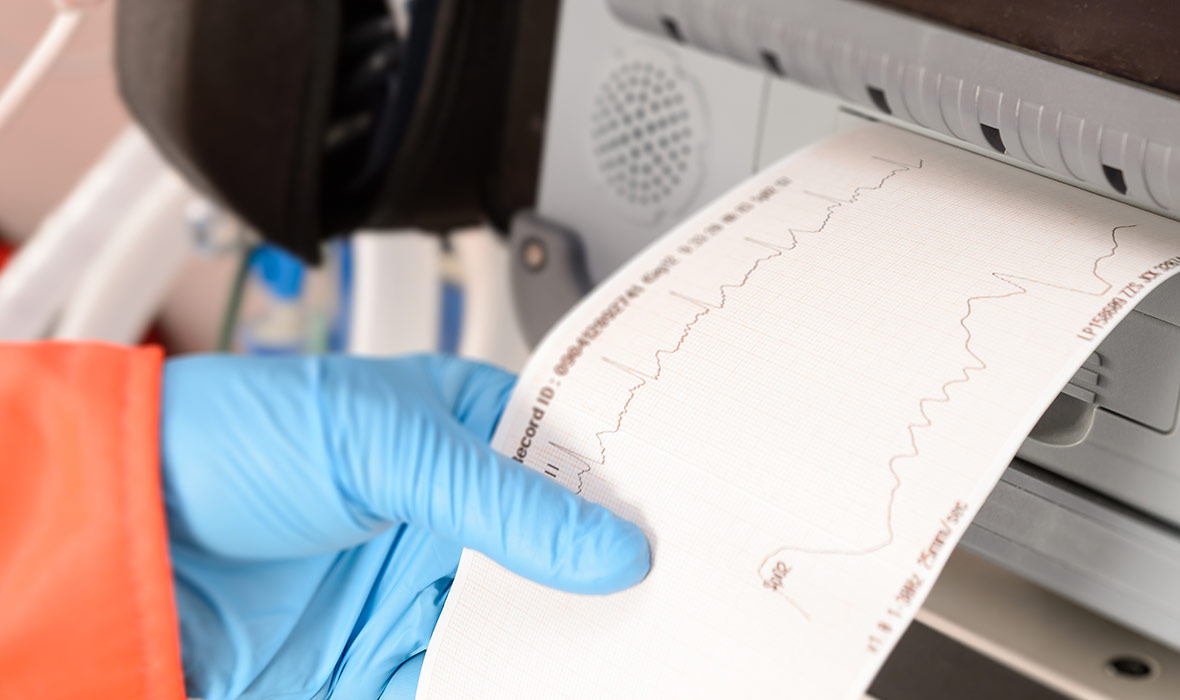
Since COVID-19 began spreading in the United States in March, emergency departments have seen a sharp decrease in the number of STEMI and stroke patients coming through their doors. For almost two months, polls and anecdotal evidence have suggested that this is happening all over the country, as well as in countries like Spain, the UK, and China. The Journal of the American College of Cardiology decided to conduct a formal study of nine major hospitals across the U.S. On April 7th, they released the results, confirming with statistical evidence what doctors have been experiencing: on average, the nine hospitals saw a 38% reduction in cath lab activations for STEMI patients.

And this trend is being confirmed in hospitals all over the nation. Dr. Jason Wasfy, a cardiologist on the Massachusetts General Hospital cardiac care unit, went an entire week without a single STEMI. “It could just be a very weird week, but it really raises a concern that patients with cardiovascular complaints or concerns may not be presenting to medical care because they’re afraid of the hospital, they’re afraid of COVID-19.”
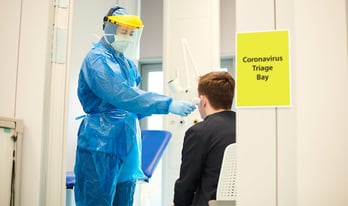 Unfortunately, it’s highly unlikely that STEMI and stroke cases are actually in decline. Doctors fear that patients are experiencing symptoms, but are delaying as long as possible before seeking treatment, out of fear of contracting COVID-19 if they head to the ER.
Unfortunately, it’s highly unlikely that STEMI and stroke cases are actually in decline. Doctors fear that patients are experiencing symptoms, but are delaying as long as possible before seeking treatment, out of fear of contracting COVID-19 if they head to the ER.
"Basically everybody stopped coming to the ER," said Dr. David Tashman, an ER physician and director of the emergency medicine department at USC Verdugo Hills Hospital in Glendale, California. "I think fear is certainly part of it. They see these images from New York, of warehouses for dead bodies behind the hospital. Everyone thinks they're going to catch their death if they show up in the ER."
Dr. Alejandro Arroliga, medical officer for Baylor Scott & White, speculated: “There was probably some fear of the unknown. But maybe people were just trying to do the right thing. They thought their condition was not so important, and they didn’t want to take a place that someone else might need.”
The national moratorium on elective surgeries and regular appointments, while necessary, has possibly also caused people to avoid seeking emergency care for as long as they can, even in areas where COVID-19 has not yet hit hard. Dr. Wasfy pointed out that there is a crucial difference between routine and emergency treatment. “Sure, a screening colonoscopy can be put off for a few months, but chest pain is a symptom that indicates an emergency and we want people to be evaluated."
Dr. Martha Gulati, editor-in-chief of CardioSmart.org, also agreed that the stay-at-home messages are not meant to apply to emergency situations. "That's a good message for the general public," she said. "But it was not intended for people with heart attack symptoms. You can't treat a heart attack yourself.”
In time-sensitive emergencies, the length of time before treatment directly correlates to the chances of a positive outcome. The longer a patient waits to seek treatment, those chances decrease dramatically.
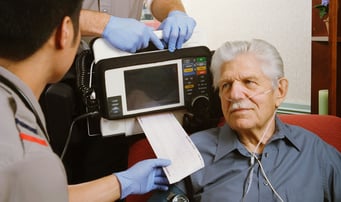 In STEMI cases, timely treatment is essential to restoring blood flow and reducing damage to the heart. In an ischemic stroke, 1.9 million neurons die every minute. And in cases of appendicitis, waiting days before seeking treatment causes abscesses and infection. “I would say 70 percent of the appendicitis on my service right now are late presentations. What happens when you present late with appendicitis is, we can’t operate on you safely,” said Dr. Evert Eriksson, trauma medical director at the Medical University of South Carolina.
In STEMI cases, timely treatment is essential to restoring blood flow and reducing damage to the heart. In an ischemic stroke, 1.9 million neurons die every minute. And in cases of appendicitis, waiting days before seeking treatment causes abscesses and infection. “I would say 70 percent of the appendicitis on my service right now are late presentations. What happens when you present late with appendicitis is, we can’t operate on you safely,” said Dr. Evert Eriksson, trauma medical director at the Medical University of South Carolina.
Dr. Tashman has seen late presentation taking a large toll on his patients. He cited three separate cases where patients were experiencing serious symptoms of a heart attack, a stroke, and appendicitis. Each waited three days before coming to the ER. "All three patients survived, but their outcomes were not as good as they could have been if they showed up earlier," he said. While fear of contracting COVID-19 is understandable, avoiding the hospital for serious conditions is not worth the damage done by waiting to seek treatment.
While the individual consequences are serious enough, doctors believe that widespread delay in seeking treatment could lead to an avalanche of ailments that are not commonly seen anymore. According to Dr. Héctor Bueno, a cardiologist in the Hospital Universitario 12 de Octubre, Madrid, “We expect to have a real increase in the number of patients who are suffering the consequences of this crisis. I suspect to see mechanical complications, cardiogenic shock, cardiac rupture, and things that we don't see that often now, that probably we will be seeing in the future.” He added, “we will probably see more post-MI angina, reinfarction, and of course heart failure and arrhythmias, as well.”
Dr. Rod Stables, a cardiologist at Liverpool Heart and Chest Hospital in England, worries that COVID-19 will be responsible for many more deaths than just the people it infected: “It is conceivable that in the UK the deaths that eventually could be attributed to COVID-19 will be dwarfed by the deaths that have occurred because of the absence of otherwise routine medical care.”
It's unlikely that we'll ever know the full extent of COVID-19's impact on STEMI and stroke patients. Hopefully, however, the coming months may provide some clarity.
 For now, though, doctors want to make sure that patients know they have a safe place to seek treatment. While ED volume is indeed high in places like New York, many emergency departments across the country have very few cases of COVID-19—if any—and are well-equipped to care for heart attack and stroke patients. Many hospitals across the U.S. are attempting to spread a message of safety, letting patients know that it’s safe to come in to get the help they need.
For now, though, doctors want to make sure that patients know they have a safe place to seek treatment. While ED volume is indeed high in places like New York, many emergency departments across the country have very few cases of COVID-19—if any—and are well-equipped to care for heart attack and stroke patients. Many hospitals across the U.S. are attempting to spread a message of safety, letting patients know that it’s safe to come in to get the help they need.
On May 4th, Baylor Scott & White Health in Dallas launched a new campaign to reassure patients that the hospital’s safety measures are working, and that the risk of catching COVID-19 within the hospital is minimal. Dr. Alejandro Arroliga, Baylor’s chief medical officer, announced that among employees exposed to COVID-positive patients, 1% later tested positive for the virus. “I honestly believe there’s a higher risk of getting the infection in the community than in our hospital,” he said. Baylor’s safety measures include UV-light disinfection, mask requirements for patients, staff, and visitors, utilizing telehealth, and hosting potential COVID-positive patients in negative pressures rooms, which can help prevent the disease from escaping.
Dr. Tashman put out a statement to reassure patients that USC Verdugo Hills Hospital is able to accommodate them, and that it’s better to come in quickly. “We've had zero cases of healthcare-acquired COVID-19, everyone is trained, we have no shortage of [personal protective equipment] and our processes are solid," he said. "So we just need to get the word out that if you're having serious symptoms, don't be afraid to come in."

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...