National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
4 min read
 Team Pulsara
:
May 01, 2020
Team Pulsara
:
May 01, 2020

On April 28th, JEMS Webcasts hosted an enriching webinar featuring a distinguished panel of EMS leaders discussing how their organizations are using mobile technology to manage the COVID-19 pandemic, and how they plan to use those same technologies in the future.
Webinar attendees heard from Dr. Stein Bronsky and Dr. Matt Angelidis, both Medical Directors for the Colorado Springs Fire Department; Chris Lester, who is the Commander of Homeland Security and Emergency Management for Austin/Travis County EMS; John Gonzales, the Commander of Clinical Practices for Williamson County Texas EMS; and Pulsara’s own Chief Marketing Officer, Kris Kaull.


The presenters gave many practical examples of how they are using Pulsara to streamline their communication processes, involve all the important players quickly, minimize unnecessary exposure to COVID-19, and come up with innovative solutions to tough situations presented by the pandemic. They also shared their vision for how they will expand their use of Pulsara in the future, extending to all types of emergency situations and Community Paramedicine.
Here are the top lessons learned in this week’s webinar:
 In the words of Kris Kaull, “A pandemic is not the best time to take something off the shelf, dust it off, and start it. Instead, using something that you use every day that can be scaled up, and then scaled back down seems to be the most appropriate.”
In the words of Kris Kaull, “A pandemic is not the best time to take something off the shelf, dust it off, and start it. Instead, using something that you use every day that can be scaled up, and then scaled back down seems to be the most appropriate.”
Ideally, you want to have a system in place that you already use on a daily basis: a platform that you and your team are already comfortable with and know how to use. It’s important to choose a platform that’s flexible enough to scale up and serve you just as well in a disaster or pandemic situation as it does for your daily needs.
Now that we’re seeing what’s possible with telemedicine, these solutions will only grow and expand. Patient privacy is still a top priority. Platforms like Pulsara are encrypted at both ends and are completely HIPAA-compliant, which will ensure the smoothest possible transition once patient privacy restrictions are tightened again after COVID-19.
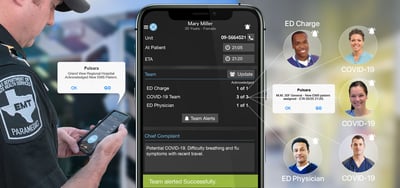
 Connecting all members of the care team on the same patient channel that is updated and viewable in real time is a game-changer. Doctors can see a patient on a video call and use that information to determine whether the patient needs to be transported to the hospital. Hospitals can pre-register patients and make more informed, intentional decisions about who needs to be on the scene when the patient arrives. Important information can be transmitted between providers: EMS can send the patient’s vitals and ECG to physicians at the hospital, and get a quick response from the doctor in real time. This minimizes errors and maximizes efficiency, which both create a better experience for the patient.
Connecting all members of the care team on the same patient channel that is updated and viewable in real time is a game-changer. Doctors can see a patient on a video call and use that information to determine whether the patient needs to be transported to the hospital. Hospitals can pre-register patients and make more informed, intentional decisions about who needs to be on the scene when the patient arrives. Important information can be transmitted between providers: EMS can send the patient’s vitals and ECG to physicians at the hospital, and get a quick response from the doctor in real time. This minimizes errors and maximizes efficiency, which both create a better experience for the patient.
For tough transport or resuscitation decisions, using a mobile platform provides a way to alert key decision makers and allow them to respond with a video call. John Gonzalez explained that in Williamson County, EMS uses Pulsara to create a new patient channel, input the type of emergency, and then send an alert to their Medical Director, so that he can initiate a video call and have the benefit of seeing the patient before advising the best course of action.
With this capability, physicians are effectively on-scene immediately, are able to see the situation firsthand, and are able to make a better, quicker, more informed decision about what should be done. Using mobile technology avoids wasting valuable time while waiting to bring everyone on the same page.

Video calls provide valuable insight that could traditionally only be obtained by being physically present on the scene. With live video, visual information can be transmitted between EMS, physicians, medical directors, and even between a medical provider and a patient.
Detailed data can be gathered without EMS even having to be on the scene. Dr. Stein Bronsky described how video capabilities are currently being used in Colorado Springs to aid a patient who needs EMS for assistance with frequent seizures and also has someone in their house with a positive case of COVID-19. Using Pulsara’s video capabilities, the paramedics can park the ambulance outside the house while being present on the scene through video. They can monitor the patient’s situation and offer emergency assistance if needed, or avoid both exposure and PPE usage when they’re able to advise from the safety of their vehicles.
Good mobile communication platforms work the same for all types of emergencies, simplifying the care coordination process, yet are flexible enough to fit each unique care team’s needs and resources.
For example, Colorado Springs is using Pulsara for video conferences with patients for follow-up care, scheduling quick consultations to check in with patients after they head home from the hospital. Williamson County paramedics can gauge whether they need to drive out to provide on-site care for patients who don’t need to go to the hospital. In the near future, they plan to test whether Pulsara can replace their radio reports altogether. Colorado Springs, Austin/Travis County, and Williamson County also have high hopes for using Pulsara to expand their Community Paramedicine programs. Mobile medicine offers a wide array of future possibilities for improving care, far beyond the scope of COVID-19.
The genie is out of the bottle; mobile medicine is not going away anytime soon. JEMS Editor-in-Chief A.J. Heightman commented, “If you’re not thinking about telehealth, you’re going to be lightyears behind [when this is all over]. I don’t think we’re ever going to go back after the pandemic. Telehealth is here to stay.”

Kris Kaull pointed out that if these technologies are available for secure use in other fields like banking, we should be able to transmit information securely in healthcare. Uniting all the different parts of the care team will result in fewer mistakes, more efficient communication, and no more time wasted on multiple calls that could be solved with one alert notification. It’s about making sure the right people have the right information at the right time, all saved and accessible in one place.
Each of the presenters expressed that they feel it’s important to use a holistic system that unites all parts of the care team. Dr. Bronsky summed it up best: “The best way to move forward, regardless of COVID-19, is a system-wide approach to advancing our communication. Everybody struggles with all these different modalities and chain links that can break. We see Pulsara as a holistic system of care that we are planning on expanding through the entire patient base, not just isolated to strokes or heart attacks. We’re already working on that and see that as the vision of our near future.”

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...