National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
5 min read
 Team Pulsara
:
Apr 27, 2023
Team Pulsara
:
Apr 27, 2023

Embracing Modern Technology Will Pave the Way for the Future of EMS Communications
On February 15th, the National Association of State EMS Officials (NASEMSO) presented a webinar hosted by Corey Ricketson, Pulsara Sales Vice President - Texas, and Eric Epley, Executive Director of the Southwest Texas Regional Advisory Council (STRAC). During the discussion, Eric and Corey discussed what it takes to build a true system of care that scales.
During the webinar, they told the story of how COVID changed Texas's approach to patient communication, logistics, and load balancing, and how creating a statewide wristband system is revolutionizing their approach to patient care and large-scale incident response.
Watch the full webinar below, and read on for the top four takeaways from the discussion!
For EMS crews in Texas, calling in patient reports became complicated by the half-face respirators they wore to protect themselves during the pandemic. Nurses on the other end struggled to hear the radio reports. As a potential solution, Texas’s Regional Advisory Councils (RACs) looked at implementing Pulsara, a healthcare communication and logistics platform. Pulsara would allow EMS to transmit patient information to the hospital without having to deliver a report over the radio. As a state, the RACs decided to move forward.
Ricketson explained Pulsara’s functionality by comparing it to a TAC channel used by EMS and fire crews for shared awareness. “Essentially, what Pulsara does is it creates a dedicated patient channel for a single patient event. As we are building that channel, any organization can start it, but the key is that they can bring in other organizations, who can then add their teams into the channel, who can then add other organizations and teams. The secret sauce is that we are all on the same communications TAC channel, but it’s within an app.”
During the pandemic, hospitals in El Paso were short on available beds. In October, November, and December of 2021, El Paso experienced a surge that left them with no available beds. To accommodate patients, they set up a field hospital in the parking lot of the University Medical Center. As the crowding worsened, they ultimately decided to load balance patients by moving them across the state.
The situation in El Paso presented a unique challenge because of the city’s distance from all the other major cities in Texas. El Paso is closer to Los Angeles than it is to Houston, which meant that in order to distribute patients across other hospitals in Texas, 300+ patients would have to be moved via fixed-wing aircraft.
The traditional patient transfer process involved many phone calls—on average, between 30 and 50 per patient. To cut down on the number of phone calls and speed transfers, the RACs used Pulsara to set up the Virtual Placement Center (VPC) with the State Coordination Office. Epley explained how the Virtual Placement Center complemented their normal transfer workflows and allowed them to pull patients through the process. “Hospitals would send their patient in Pulsara to the Border RAC, they call it the RMOC (Regional Medical Operations Center) in El Paso. The Border RAC would check with other local hospitals and the alternate care facility. If they were inundated and couldn’t accept the patient, then the patient was [entered into] something we call the Virtual Placement Center with the State Coordination Office. The State Coordination Office’s coordination center would send those patients to all the other RMOCs, and they would socialize it, and you could accept the patient from the Virtual Placement Center in the software. This eliminated almost all of the phone calls.”

The coordination didn’t stop there; as the patient was moved to the receiving facility, care team members used the Pulsara channel to keep an open dialogue. Epley explained: “Once the jet was dispatched to go to the call, that crew was on [Pulsara], and the receiving hospital was seeing what was going on as people put patients in. [They would] put in, ‘Hey, we just landed at the airport, we’re on the way to the hospital.’ It was just so much richer understanding about what was going on with those transfers. It was very helpful.” With the VPC, they were able to successfully arrange transfers for all 300+ patients.
Ricketson commented on how the new system's efficiency reduced the number of phone calls required, freeing up time and improving communication. “Having shared awareness through a single channel with all the people who had a vested interest in that patient’s movement, care, or logistical needs, really got rid of all those phone calls.”
Following the situation in El Paso, emergency leaders in Texas realized that muscle memory is the key to a successful approach to emergency management. In a disaster, everyone’s first instinct is to turn to how they’re used to doing things. Pulling a solution off the shelf that’s only used on rare occasions sets everyone up for failure, as no one is accustomed to using it. Epley summarized it best: “If you don’t use it every day, you’re not going to use it on disaster day.”
The definition of building a system of care that scales is using the same system daily to build muscle memory. That’s the philosophy behind Pulsara’s patient tracking capabilities. When first responders and EMS crews are accustomed to using Pulsara every day for every patient, the same workflow will apply for triaging and tracking patients during a crisis.
Before the pandemic, Texas was working to develop statewide wristbands to be used across organizations. After speaking to data experts, they realized that the secret ingredient to successful patient tracking was to create one wristband that would be used universally across the state. That wristband could then function as a universal ID for the patient, no matter which organizations participated in treating them.
At the time, Pulsara was working on driver’s license scanning, and Epley asked if it would be possible to use the same workflow to scan the Texas wristbands and populate the ID in patient channels. Pulsara updated the software to add the capability. Now, providers can scan patient wristbands to create a new patient channel or locate an existing one.
The workflow involves minimal data entry. Ricketson demonstrated how to scan the wristband to create a new patient channel, scan the patient’s driver’s license to enter information such as name, age, and DOB, take a few pictures of the patient, their injuries, and their belongings, and then use talk-to-text to enter the information that would normally be delivered in a radio report. Everyone along the care journey who scans the patient’s wristband to join their channel can see all the information.
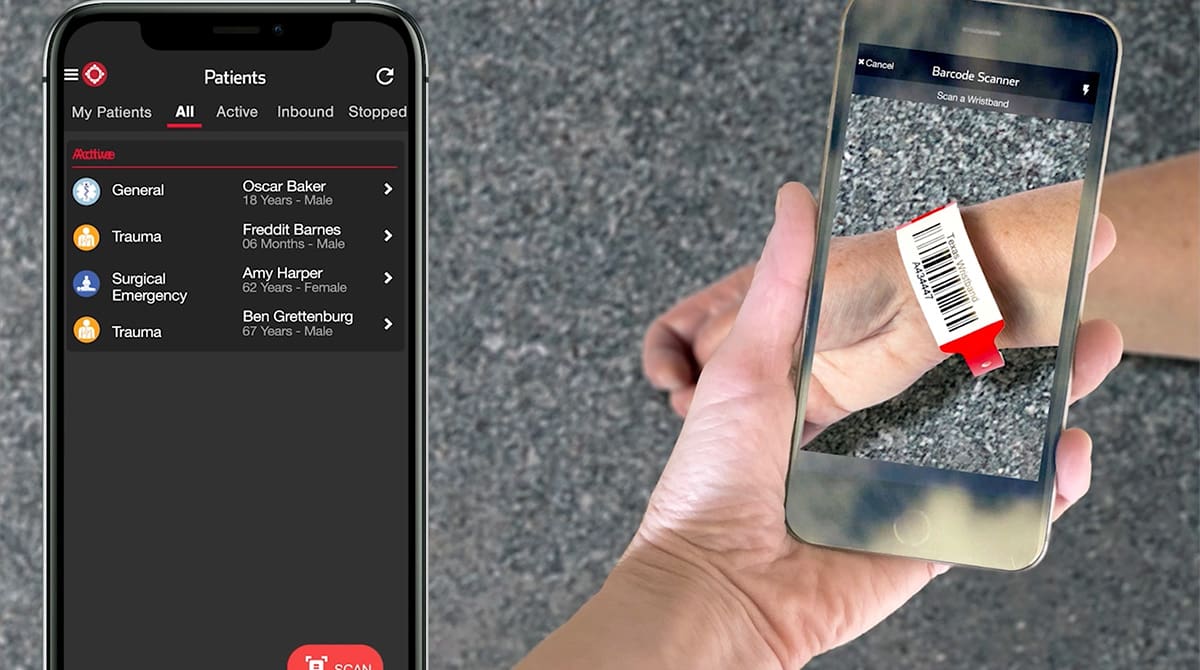
The Texas statewide wristbands promise to revolutionize patient tracking during large-scale emergencies. Paired with Pulsara, the wristbands now make it possible to track patients across organizations. First responders on the scene can put wristbands on patients and use Pulsara to scan the wristband and create a patient channel for them. As other providers encounter the same patient, they can scan the wristband to access the patient's channel, see the information that's already been added, and contribute to the conversation. Responders can add photos of the patient and their belongings to assist in reunification.
Texas is working towards using the bands for every patient on a daily basis. That way, ambulances will already have the wristbands handy when disaster strikes and will be comfortable using them. “Everyone has a mobile device that we use every single day,” Ricketson said. “If we put the wristbands on every single patient, whether they’re experiencing toe pain, chest pain, trauma, etc. —then, when we have a disaster, it’s no different. Every day is disaster day.”
Want to learn more about patient tracking with Pulsara? Check out Patient Wristbands + Pulsara.

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...