Pulsara Around the World - June 2026
April & May Recap A Decade of Proven ResultsOver the last decade, 20 third-party, peer-reviewed research studies have demonstrated Pulsara's clear...
4 min read
 Team Pulsara
:
May 28, 2021
Team Pulsara
:
May 28, 2021

EDITOR'S NOTE: Special thanks to Brandon Means for writing today's blog post. Brandon worked at Pulsara for over a decade, ending his tenure as Pulsara's Senior Vice President of Medical Operations in 2026. You can connect with him on LinkedIn.
—
The patient care report is one of the most crucial parts of a call. This is your chance to give the hospital a brief report about your patient and let them know that you're on your way, giving them time to prepare for your arrival. Typically, though, you have to deliver your report in the midst of a chaotic scene, and things are equally as hectic at the hospital. What information is essential to communicate to the hospital before arrival?
Pulsara's Vice President for the Western Region, Brandon Means, teamed up with EMS1 to produce an original video series of critical paramedicine tips and techniques, called Progressive Paramedic. In this week's video and blog post, we throw back to Brandon's paramedic days as he reviews the three essential elements of a good patient report. Check it out below!
Let's think for a second about how we communicate on a daily basis with our friends, our family, our coworkers, and then let's apply that to healthcare.
Your spouse calls you, trying to read off the grocery list. About 10 items into the list you say, "Stop, just text it to me." Right? Why do we do that?
It's hard to pay attention and retain details when there are many distractions around. So let's apply that to the EMS world—and more specifically, the patient report. We're in the back of an ambulance, transporting a patient to the hospital. You're three minutes into the most amazing report you've ever given. You finally finish the report, and what do you receive as the response?
"Room assignment on arrival."
We can hope that they were able to write down a couple of important pieces of that report while the chaos was going on around them, but really we're at the mercy of the person with a pen on the other end of the phone.

Miscommunication between caregivers is one of the leading causes of medical errors in the healthcare field. The vast majority of these happen during a transition of care—meaning from EMS to the ER, or from the ER to the ICU. That's why it's so important that we effectively communicate during these key times in the transition of care.
So how do we ensure that we effectively deliver the pertinent information accurately? Let's examine the contents of our patient reports and identify the three things that hospitals need to gather from each patient report.
The first piece of information the hospital needs to gather from our patient report is whether the patient is stable or unstable. They need to know this for a couple of reasons; first, so they can prioritize incoming traffic and put the patient where they need to go. The second reason is so they can mentally prepare for a patient that may be coming in that's unstable.
The second thing the hospital needs to know is, do they need any additional resources? If you went to EMT school back during the days of BTLS, you probably remember your scene size up: how many patients do I have? Are there any additional resources that I need? This is the same for hospitals.
So if you're bringing in a patient who is on a ventilator, they're going to need to know that they need to gather a vent and probably a respiratory therapist. If you're bringing in a violent patient, they probably need security at the bedside. They need just enough information to determine any other resources they may need, such as multiple infusions, or they may need to gather some more pumps. Let's make sure that those pieces of information—the pertinent things that they need to know to prepare their team—they're getting from us.

The third piece that really needs to be gathered from our patient report is: where does this patient need to go? Does this patient need to go to an ER room? Or is it a patient that needs to go through the ER? As we know, there's a small subset of our patients that need to go through the ER, rather than sit around in the emergency room. Some examples are STEMI or stroke patients who really need to be on a cath table or in a CT table. We need to get that pertinent information to the hospital so that they can effectively mobilize the proper teams.
As always, follow your local protocols and guidelines when it comes to patient reports.
As an industry, we need to be constantly evaluating and improving the way we do our job. And a big part of our job is communication. We should constantly be asking: is there a better way?
The traditional radio report has served us well for a long time, but now, there are newer and faster methods of getting all these same pieces of information to the entire hospital care team at once.
We can use mobile technology to leverage HIPAA-compliant communication platforms like Pulsara. These solutions offer us the opportunity to notify the hospital with more detailed patient information, including demographics, vitals, photos, notes, audio clips, and instant messaging. That way, we can communicate the right information to the right team members at the right time, which gives them more time and more information as they prepare to treat our patients.
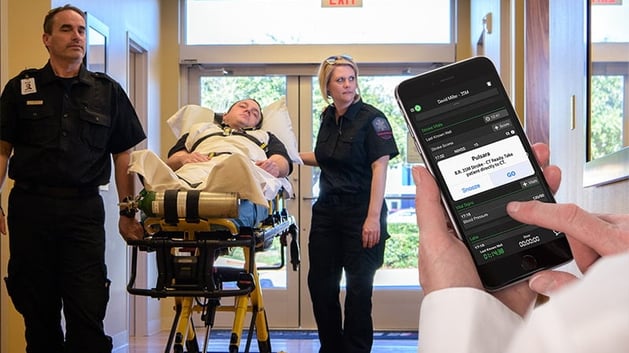
Want to know how you can replace the traditional radio report with Pulsara? Learn more here.
Editor's Note: This post was originally published in August of 2017 in collaboration with EMS1 and has been refreshed and updated for accuracy and comprehensiveness.
![]()
While it’s critical that EMS providers stay on top of the latest clinical skills for saving lives, it’s also important to look for ways to improve overall operations. Check out our free eBook to learn more.

April & May Recap A Decade of Proven ResultsOver the last decade, 20 third-party, peer-reviewed research studies have demonstrated Pulsara's clear...

National EMS Week continues today with EMS Recognition Day, a time to honor the paramedics, EMTs, dispatchers, and emergency medical professionals...

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...