Pulsara Around the World - June 2026
April & May Recap A Decade of Proven ResultsOver the last decade, 20 third-party, peer-reviewed research studies have demonstrated Pulsara's clear...

Editor's Note: On August 11th, EMS1, Fitch & Associates, and the National EMS Management Association released their fourth annual EMS Trend Report, proudly sponsored by Pulsara. Because the articles and advice found within contain such critical subject matter, we've elected to publish each segment one at a time here on our blog. Read, enjoy, share, and take to heart the following information brought to you by the most prestigious thought leaders in EMS. This fifth and final entry in the 2021 Trend Report is written by Rob Lawrence, director of strategic implementation of PRO EMS Cambridge, Massachusetts, and executive director of the California Ambulance Association.
After a tumultuous year, we anticipated some shifts in the 2021 EMS Trend Report. We did not see a major shift in levels of burnout, or why providers are leaving their agencies, as we may have expected. What we did see, however, was a change in the three most critical issues facing EMS today. In a shift from 2020, provider mental health and provider safety rounded out the top three critical issues, behind retention of quality personnel, which has remained consistent.
The 2021 EMS Trend Report survey revealed a lot about respondents’ opinions regarding their safety and well-being. Views on and requests for support for mental health of both providers and their patients were telling, as was the need to offer physical and personal protections, both on the person and in the vehicle.
After examining the key responses in the safety arena, issues identified and possible solutions, as follows are eight areas in which Trend Report respondents are asking for safety improvement.

Many Trend Report respondents are concerned about the workload management in their organizations. It has not only been during the pandemic where demand has exceeded the supply of both ambulances and staff, and this issue can be partly solved through recruitment and retention initiatives. We are all aware of the shortage of EMTs at this time and without that additional staff in the right geographical location, then field crews will continue to feel the pressure. We are painfully aware that the precarious state of EMS reimbursement hinders the ability to pay more, but continued work by our national associations continues to raise this issue that, if not fixed, could end up with the whole EMS industry becoming the fatality.
An additional stressor on the system is the use of red lights and sirens to respond to a call. This has been the subject of continuous study and opinion. There is a firm belief that it is not necessary to drive hot to every call, however, many local agreements and contracts require this to happen. The risk involved in continuous red lights and siren operation place the provider, the patient, and the pedestrian at risk, and rationalization of what is worthy of an emergency response versus operating under normal road conditions is required. This will take input from local politicians, policymakers, chiefs, medical directors and, most importantly, staff. Many of our national associations agree that the use red lights and sirens is being overused and are speaking out on this issue with ever-increasing volume.
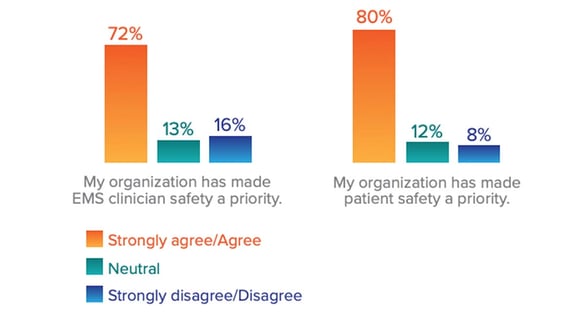
For well over a decade now, the value of establishing a culture of safety in an agency and employing the principles of crew resource management have been emphasized. Comments in the Trend Report survey identify that for some agencies, this is still either a work in progress or nonexistent. For those that still have this on the to-do list, it must start at the top, in the corner office, and pervade down through the organization, so all feel comfortable and supported. The key measure in this lies in the confidence of the most junior member of the organization in feeling comfortable speaking up when something is not right or to volunteer an error without fear of punitive action. How would your organization fare in this test?
The Trend Report results also highlighted the need to ensure all staff are fully and appropriately trained. One respondent noted that recruits have little-to-no life experience, and lack the knowledge and awareness required for entering a potentially dangerous situation. It is incumbent upon an organization’s leaders to ensure that new staff are educated to operate in the environment in which they are about to be employed.
Respondents weighed in on the education level and age qualification; however, the overarching question of merit course, associates or bachelor’s degree remains an emotive subject and requires further work, understanding and cooperation at the national level.
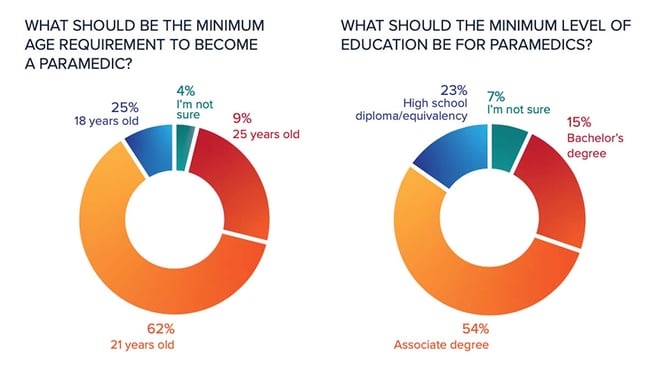
Returning to training versus education, the onus is on the individual agency to train a fit-for-purpose, clinically sound and resilient provider. One area that merits attention is that of driver training.
We do not want to be mere “ambulance drivers,” but, unfortunately, we must get ourselves to the patient and the patient to the hospital. This requires an element of professional, safe, and skilled vehicle operation involving the whole crew to drive, navigate and communicate without distraction or accident.
Vehicle accident rates and the images of ambulances splayed across our streets, while EMS is not always at fault, indicate we must work harder in the training and orientation phase.
A major issue, both in the survey results and in EMS, is that of provider well-being and mental health. The pandemic has taken our profession to the edge and often beyond, and the requirement to offer pastoral care to our workforce has never been more important. Every organization should have EAP programs, as well as critical incident debrief teams to ensure that we care for the caregivers. Many organizations are employing or affiliating with local chaplains to offer non-denominational caring ministry to workers, and this has been very well received. Chaplaincy offers a non-chain-of-command ear to listen to problems, offer guidance and support, and pass concerns up to those that would otherwise be unaware of issues in the workforce.

The mental health of our patients also gives cause for concern. The EMT and medic in the current environment often must act in the role of social worker, mental health specialist and the calm voice of de-escalation. This requires more training than is currently delivered across any national syllabus, and classes such as critical incident training should be considered.
Also, after the events of the last year and potential reductions in police availability, concern exists for provider safety as the previous and traditional ring of law enforcement protection may well be either delayed or nonexistent. This is a major issue that requires the navigation of local policies and politics to ensure staff are safe to go about their responding business.
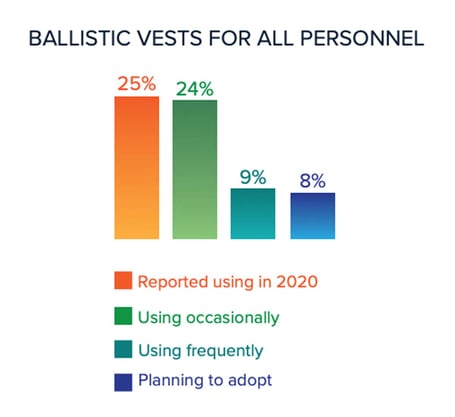
Physical safety is also a major concern. The question of ballistic protection was also raised. The threat to our providers requires protection, particularly for those who operate in tactical scenarios, but for those who want to wear body armor, the old soldier in me says that you must acknowledge that the threat is asymmetric, and you do not know where the attack will come from.
Therefore, if vests are issued, then they must always remain on. To say that one can discern when this level of protection is needed is perhaps naive as the assailant attacks at a time and place of their choosing and not ours. That said, some degree of self-extraction training may be something to consider as well as a body-worn camera, which offers quality assurance/quality improvement feedback, as well as evidence in the event of an assault and may even act as a deterrent.
As we roll out of 18 months of the pandemic, we are all tired. The strain has been unhealthy and leaders at all levels must monitor the levels of fatigue in the workforce. High unit hour utilization, record call volumes and emotional distress cause fatigue. This, in turn, leads to accidents and errors or burnout. Shift length has been the subject of much debate in the past. For 24-hour shift work, while good for accumulating time off, the fatigue associated with raised call volume and little downtime is potentially fatal and must be addressed. As a minimum, breaks must be managed, and napping allowed.
Musculoskeletal injury is a major ailment that affects EMS providers, and many medics can remember the day their back “went.” Given an enhanced push for better back care, there are now many mechanical aids in the marketplace to safely lift patients.
Ask any EMS chief or HR director and they will tell you that before the pandemic, the main injury that caused high levels of worker’s compensation was associated with lifting injuries. Responses in the Trend Report note that increased access to power loading systems and self-raising stretchers would aid both safety and patient handling. Unfortunately, like all EMS equipment, it doesn’t come cheap and sticker shock may inhibit some from making large capital purchases. It is highly recommended to search for alternative methods to ease the cost. Every year, the Assistance to Firefighters Grant offers millions of dollars, but many are unaware that an element of that funding is preserved for EMS purchases.

In my time as COO of the Richmond Ambulance Authority, we were successful in an AFG application and received $320,000 to fully re-equip our fleet with Power Pro stretchers. The justification in the paperwork – the downtime caused by back injury. Quite simply, lifting patients is hazardous to provider health and any device purchased to assist is truly an invest-to-save initiative.
To address survivability in an ambulance crash, the design of your workhorse vehicle must be seriously considered. If we follow the European CEN standard of ambulance construction – rules that govern the design spec safety considerations and even color of an ambulance – then we should immediately outlaw the bench seat in favor of forward-facing (with the ability to turn for patient care) seats. The recurring argument is that a bench seat could hold a patient on a backboard to increase capacity at a major incident. Ask yourself how many times that has happened, versus vehicle collisions where the occupants of the rear compartment have been thrown around the back because they weren’t secure.
Safety of both personnel and equipment is a responsibility that begins at the top. It is also
the place where safety culture should emanate from. The key issues raised in the EMS Trend Report must be monitored and, if not functioning properly, changed.
Failure to care for the well-being of staff hits morale, which has downstream consequences for patient care, retention and reputation. Failure to secure the environment and equipment that we operate with will result in incidents, accidents and most probably a disaster, and nobody wants that.
Download the full 2021 EMS Trend Report
About the Author
Rob Lawrence is director of strategic implementation of PRO EMS Cambridge, Massachusetts, and executive director of the California Ambulance Association. Rob is also the principal of Robert Lawrence Consulting. Previously, Rob served as COO of the Richmond Ambulance Authority.
Rob is a former board member of the American Ambulance Association and currently serves as chair of its Communications Committee and a member of the media rapid response task force.
Pulsara is helping with COVID-19 management by helping mitigate patient surge, streamlining patient transfers, minimizing exposure, and more. Learn more about COVID-19 + Pulsara here.

April & May Recap A Decade of Proven ResultsOver the last decade, 20 third-party, peer-reviewed research studies have demonstrated Pulsara's clear...

National EMS Week continues today with EMS Recognition Day, a time to honor the paramedics, EMTs, dispatchers, and emergency medical professionals...

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...