National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
2 min read
 James Woodson, MD
:
Mar 21, 2017
James Woodson, MD
:
Mar 21, 2017
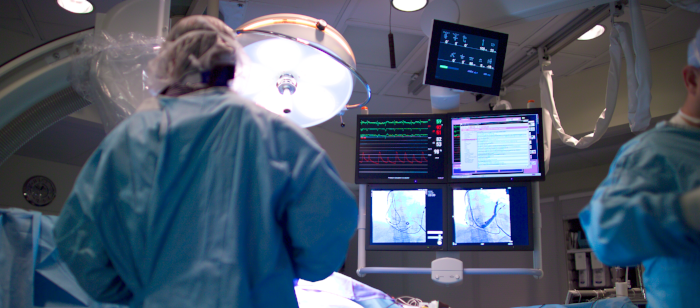
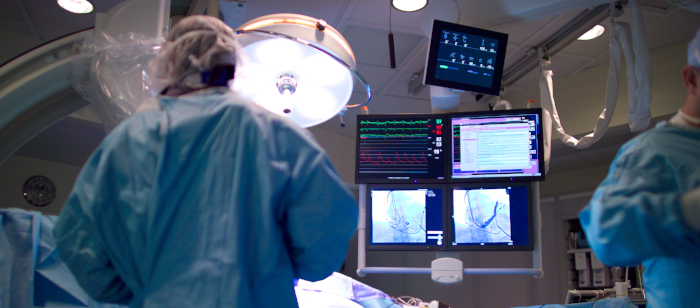 There's still much to learn about appropriate identification and triage of our stroke patients, but it is also important to understand what we can do NOW.
There's still much to learn about appropriate identification and triage of our stroke patients, but it is also important to understand what we can do NOW. Bridging therapy made functional independence equally likely for stroke patients transported first to primary stroke centers without endovascular capabilities and peers taken straight to a comprehensive stroke center, a study showed.That strategy of IV thrombolysis within 4.5 hours of symptom onset at one center followed by transport to another where mechanical thrombectomy can be performed within 6 hours of symptom onset was just as likely to produce good functional outcomes 3 months later (modified Rankin scale scores of 2 or below) as transporting patients straight to a thrombectomy-capable center (61.0% versus 50.8%, P=0.26) -- even after multivariable adjustment (P=0.82).
"This study found that patients treated under the drip-and-ship paradigm also benefit from bridging therapy, with no statistically significant difference compared with those treated directly in a comprehensive stroke center," Sonia Alamowitch, MD, of Hôpital Saint-Antoine in Paris, and colleagues reported online in JAMA Neurology.
>> Continue reading.
In the article, Louis R. Caplan, MD, of Beth Israel Deaconess Medical Center in Boston also recommended several changes to all stroke centers:

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...