National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
2 min read
 Team Pulsara
:
Aug 05, 2019
Team Pulsara
:
Aug 05, 2019
Improving quality of care and outcomes for stroke patients goes beyond the decision to give tPA. It's about communication and coordination among ALL members of the care team to save time when even seconds matter. Here are seven tips to improve quality of care for stroke patients.
It’s simply essential. Too many hospitals choose not to allow EMS to activate a stroke prior to arrival. This mindset wastes time that the hospital could have been using to pre-register the patient and activate the cath lab.
The medics must obtain a thorough history and begin preparations for tPA. Today's most successful systems use telemedicine technology for real-time video consultation with the hospital team members while still en route.
Even those systems that follow tip number 1 and regularly allow pre-notification often have room to improve -- it's imperative that the pre-notification results in all team members involved in the patient's care being brought together on the same page, and that steps are immediately taken to reduce time-to-treatment. While the ability to build and change the care team on your communication platform should be dynamic on a case-by-case basis, below is a list of those who should typically be notified as soon as the stroke is called in:
With some advanced warning, CT can have the table cleared so the patient can move directly from the EMS stretcher to the CT table without stopping at the front door for registration. Instead, registration can meet the patient in radiology. (NOTE: If your protocol mandates the patient stop in the ED, putting the patient on a portable monitor will save a couple of minutes when you leave for CT).
We all know that the time-limiting step is CT, making it important to minimize other steps before the CT as much as possible. Remember, a more detailed assessment can happen after the CT is complete.
If the neurologist is there, the ED physician can split off and start talking with the family to gather crucial pieces of information, including:
Endovascular Today stated that "Historically, interfacility transfers for ELVO have been inefficient and have resulted in a substantial percentage of futile transfers." BUT, they indicated that "It is possible to develop a more streamlined transfer process for thrombectomy. One such successful protocol focuses on three key elements:
Early vessel imaging at the initial hospital;
HIPAA-compliant, cloud-based image sharing with the stroke team at the receiving facility; and
Whatever communication technologies your team uses to coordinate care for ELVO stroke, ensure that they instantly connect ALL players -- from EMS to various departments at your hospital to key players at facilities outside of your hospital -- in one place where everyone can see all the imaging, data, patient information, and case progression. (See how Pulsara + stroke could support your teams). ![]()
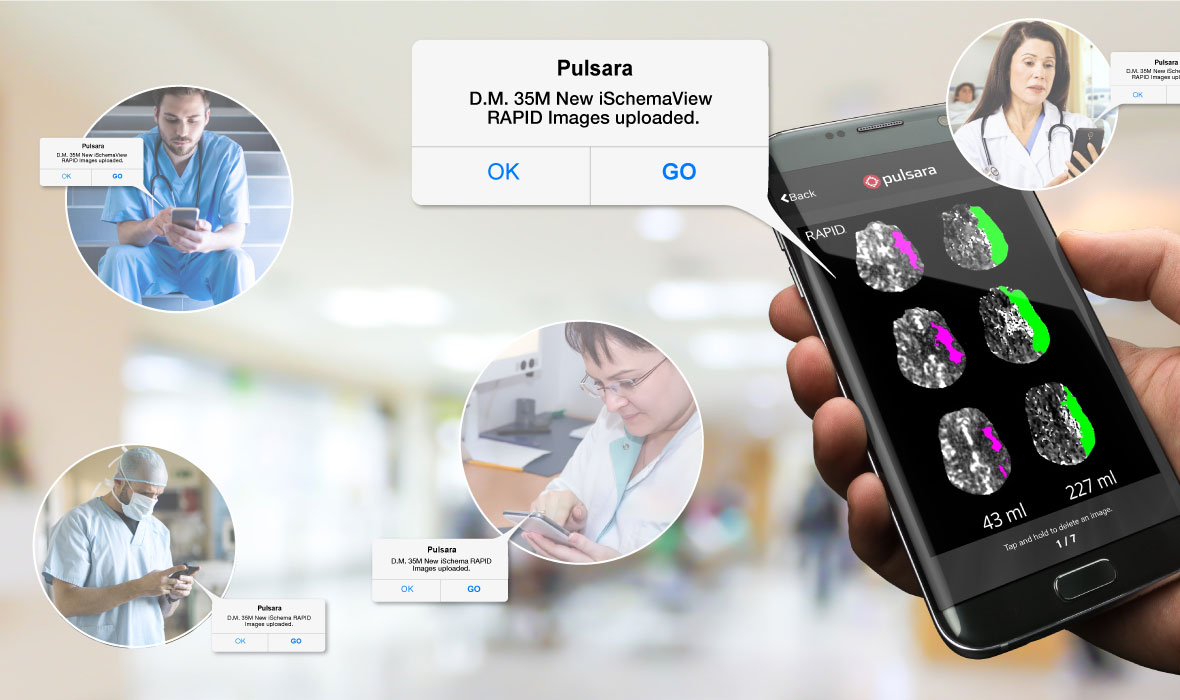
Did you know Pulsara integrates with iSchemaView RAPID to allow real-time sharing of RAPID images, including CTP, MRI, and CTA? Learn more here.

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...