National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
3 min read
 Team Pulsara
:
Oct 01, 2019
Team Pulsara
:
Oct 01, 2019
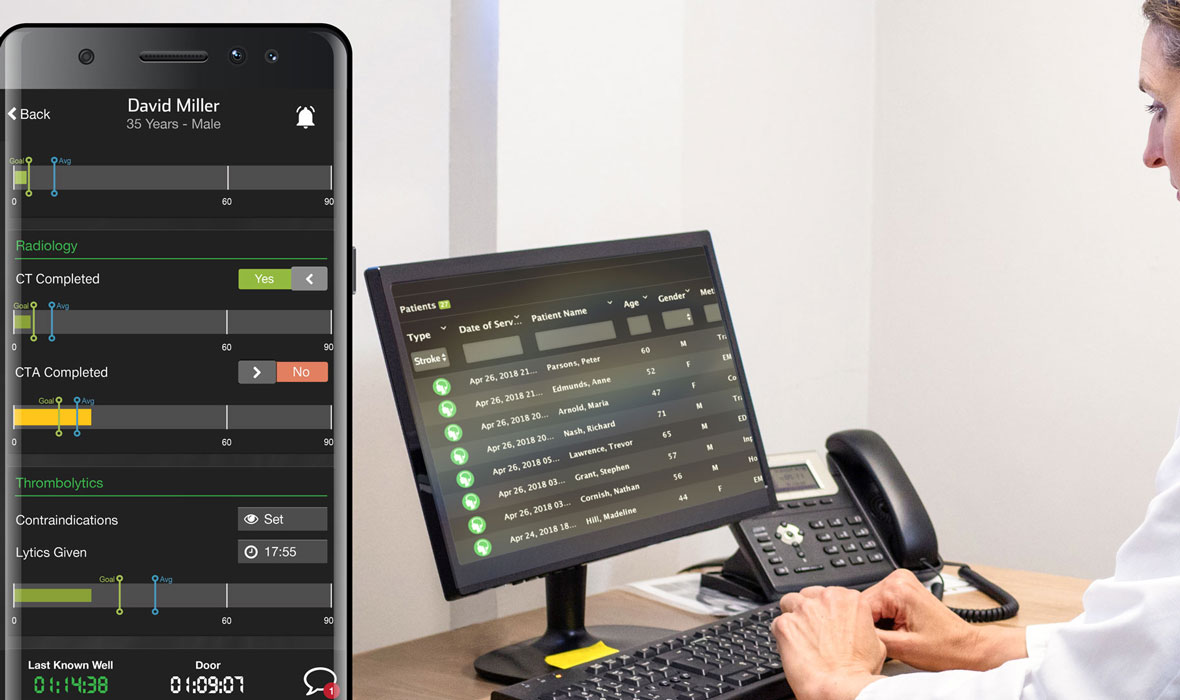
One of the biggest contributors to inefficiency in healthcare is a lack of communication, which can lead to lower quality of care and higher costs. Communication in healthcare is siloed for many reasons, including the complexity of the work, the size of health systems, outdated and non-integrated communication technologies, and HIPAA constraints.
"We do really well inside of each team [in terms of communication] … but when we try to cross those disciplines, or actually go between facilities, we start to see a breakdown or dissolution in the quality of information," said Forrest Winslow, clinical specialist at health IT company Pulsara.
In a webinar sponsored by Pulsara and hosted by Becker's Hospital Review, Mr. Winslow and Seattle-based Virginia Mason Medical Center's Director of the Emergency Department/Observation Unit Rea Berg discussed some of the challenges of improving communication in healthcare and how technology can help.
Technology has fundamentally changed the way we communicate in our daily lives. From e-commerce websites to ride sharing apps, communication is largely relegated to our smartphones, mobile devices and laptops. Since we are growing increasingly comfortable communicating via mobile technology, Mr. Winslow suggested healthcare communication could be vastly improved by implementing technology that mirrors that which we use in our daily lives.
Deploying the right tool
A comprehensive, mobile communication tool that gives all relevant providers visibility into a patient's journey has helped Virginia Mason Medical Center improve key quality metrics, said Ms. Berg.
The hospital deployed the HIPAA-compliant Pulsara communication tool in August, 2018. Initially, it was only used for stroke patients that were brought in by emergency medical services teams.
Here is how it works: when EMS picks up a stroke patient, they activate the case via Pulsara, alerting the ED staff at the appropriate hospital. At this point, a care team member at the hospital, typically a registered nurse in the ED or charge RN, can send the alert to all appropriate providers within the hospital to let them know that a patient is on their way.
This allows the hospital to get its teams in place, so that as soon as the patient comes in, action can be taken quickly and efficiently. The tool enables all those with access to follow the patient's journey, as they are taken from one section of the hospital to the other, so that clinicians know where and when they may be needed. The tool also allows providers to ask questions and receive answers in real time, ensuring the most up-to-date information is available for all involved.
Before deploying any new tool or process at Virginia Mason, all the teams involved are briefed and have a chance to give feedback, said Ms. Berg. It is important to talk with the team and connect the dots for them in terms of the 'why' behind the change and potential benefits.
"Showing them how they will literally save time and … [have good] outcomes was key," she said.
How the tool changed workflow
Prior to Pulsara’s implementation, the workflow at Virginia Mason's ED was linear, moving from one process to the next in a step-wise fashion. The platform's implementation allowed for processes to be completed in parallel, saving time when it matters most.
The tool also enabled the creation of individual alerts, allowing caregivers to discuss treatment plans for specific patients in real time.
"It created a true team culture because everyone really saw what they were working [with]… and removed the silos," Ms. Berg said. "And then at the end, we saw the impact it had on our cases."
One of the biggest changes in terms of metrics at Virginia Mason was the change in its door-to-groin puncture times for stroke patients. When the Pulsara tool was first implemented in 2018, the hospital's door-to-groin puncture time was 150 minutes. By August of this year, that time was down to an average of 89 minutes, a 40 percent decrease.
Additionally, in 2019, the median door-to-CT scan time dropped from 17 minutes in June and July to 14.5 minutes in August with use of the tool.
The Virginia Mason team also used another time-saving feature of the tool — the ability to create pre-scripted messages. These include messages that are commonly used, such as "patient CT negative," which are templated and included in the tool so that caregivers don't need to waste time typing out these common messages, said Ms. Berg.
Pulsara also helped close the loop with EMS teams, who may want to know what happened to patients they brought in. The team at Virginia Mason is able to use the tool to gather the relevant data easily and pass it on to their EMS teams.
Future steps
Pulsara has several dedicated workflows, including stroke, STEMI, trauma, cardiac arrest, sepsis and general patient. In addition to the stroke module, the Virginia Mason team recently implemented the STEMI module. The hospital is looking into using the tool for neurosurgery and in the operating room next.
Additionally, hospitals and EMS teams in and around Seattle are planning to deploy the Pulsara platform in the next year. This will open up the possibility of more efficient inter-facility communication across the city. It will also allow hospitals and EMS teams to come together and compare data to find areas of opportunities for further improvement in care coordination.
"[It's] breaking down silos in a regional manner and truly doing the best thing for the patient and providing superb care," Ms. Berg said. "I think it will move our region to an even higher level of performance with what we are doing for our patients."
View the full webinar here:

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...