National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
2 min read
 Team Pulsara
:
Apr 20, 2016
Team Pulsara
:
Apr 20, 2016
EDITOR'S NOTE: Special thanks to Brandon Means for writing today's blog post. Brandon worked at Pulsara for over a decade, ending his tenure as Pulsara's Senior Vice President of Medical Operations in 2026. You can connect with him on LinkedIn.
—
Defining Sepsis and Septic shock has been a hot topic since 1991, when the first definitions and clinical criteria for these conditions were published. After Emmanuel Rivers published “Early Goal-Directed Therapy in the Treatment of Severe Sepsis and Septic Shock” in 2001, the Surviving Sepsis campaign kicked off, significantly increasing awareness of Sepsis.
Since then, the consensus definitions of these conditions have changed multiple times. The question to ask is “Are we improving patient outcomes by changing the definitions?” If better defining syndromes like sepsis and septic shock is translating into adopting new treatments that benefit patients, it’s important that we stay up to date on these consensus definitions.
In 2001, the definition of sepsis (Sepsis-II) was simplified to the presence of an infection plus SIRS (systemic inflammatory response syndrome). Septic shock was defined as severe sepsis that was refractory to fluid therapy.
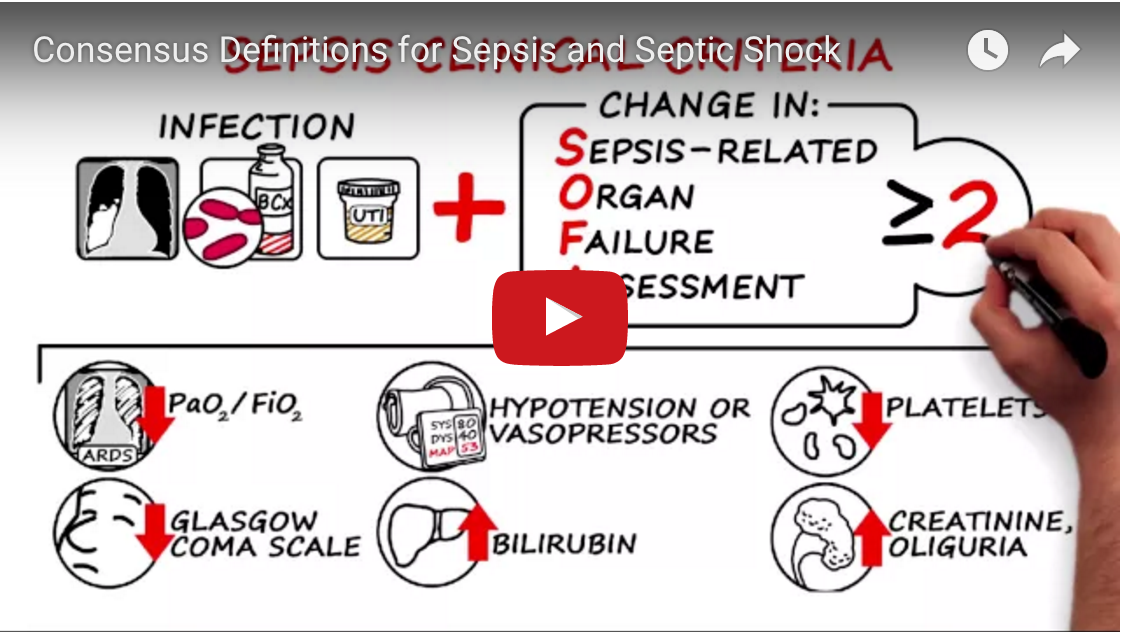
Now, in 2016, the third consensus definitions of sepsis and septic shock (Sepsis-III) have been published (see the differences between Sepsis-II and Sepsis-III here). When compared to the Sepsis-II definitions, the Sepsis III definitions replace the presence of SIRS with the SOFA (sepsis-related organ failure assessment) score. For areas outside of the critical care environment, a quick bedside score (qSOFA) is recommended.
When comparing the new consensus guidelines (Sepsis-III) to the old guidelines (Sepsis-II), there are a few things to consider. It may be a stretch to label the new definitions a “consensus,” at least in the United States. While the Sepsis-III definitions have been endorsed by the Society of Critical Care Medicine, the American Thoracic Society, and the Association of Critical Care Nurses, they have not been endorsed by the Infectious Disease Society of America, let alone any of the Emergency Medicine or Hospital Medicine Societies. Since sepsis is most often identified and diagnosed by an ED Physician or Hospitalist, this is hardly a consensus (according to PulmCrit).
What we do have a consensus on is the fact that defining and diagnosing syndromes like sepsis is, and should continue to be, a dynamic process that continuously evolves with new research. Since there is no magic number, lab value, or diagnostic tool to diagnose sepsis, knowledge of evidence based criteria, and willingness to challenge the status quo with new ideas and technology is key in improving patient outcomes.
For a detailed look at the new definitions, check out this video:


National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...