National Nurses Day: Celebrating Nurses Everywhere
National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...
EDITOR'S NOTE: Special thanks to Brandon Means for writing today's blog post. Brandon worked at Pulsara for over a decade, ending his tenure as Pulsara's Senior Vice President of Medical Operations in 2026. You can connect with him on LinkedIn.
—
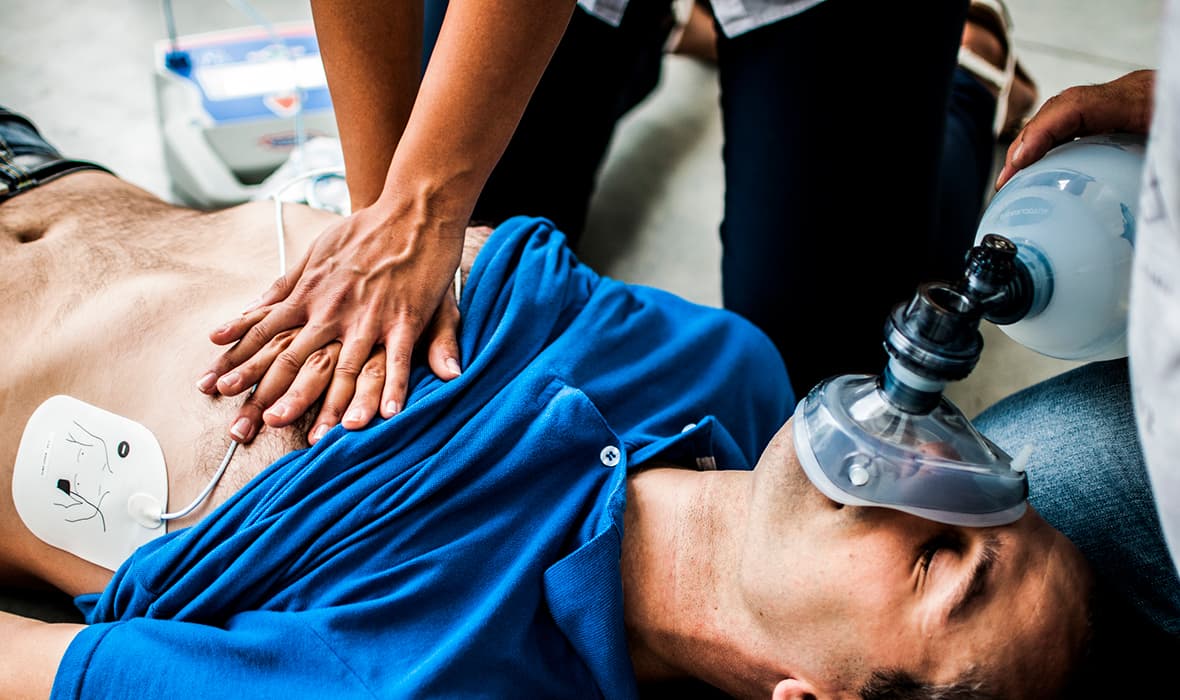
Airway management is the set of procedures and techniques medical professionals use to ensure that a patient's breathing pathway does not become obstructed if at risk or to clear the airway if already obstructed. It is a critical, life-saving skill all medics must be well-versed in.
But when should you manage a patient's airway? And why should you do it one way vs. another way?
Today, we're going to talk about airway management. Now, airway management is always a hot topic in EMS. But instead of focusing on how to manage an airway, today we're going to look at the why and the when, which is a very critical component of the big picture of airway management. I'm sure we've heard the terms a million times—less than eight, intubate, or there's some magic number or formula to gauge when we should intubate someone. Today, we're going to look at the three indications that someone needs an advanced airway.
Luckily, today we have many more tools to manage an airway than we did years ago. And when I say years ago, I'm talking about the days before RSI, noninvasive positive-pressure ventilation, and then, of course, multiple supraglottic airways. So before we dig into that tool belt, let's look at these three indications on why and when we need to manage an airway.
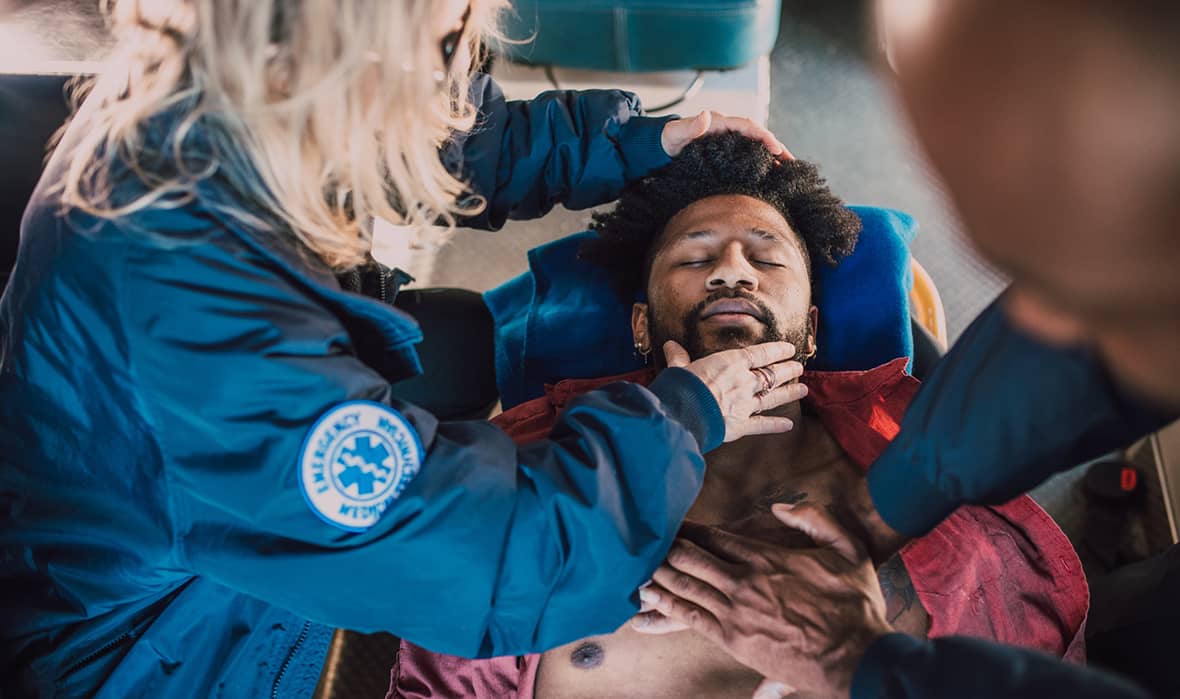
Number one is the inability for the patient to protect their own airway. Now, for years, we said if the patient's GCS was less than eight, we intubate, or there was a hard number that we would follow. Or many times, my personal favorite was if they have a gag reflex, we don't intubate. And if they don't have a gag reflex, we would intubate. We've learned now through science that that really is not a good indicator of airway management. What we really want to look at is if the patient can either spit secretions or swallow secretions on their own. And if they can, chances are they can manage their own airway. If they can't, then there's a good chance that we're going to need to take control of their airway for them, whether that's with RSI or another method.
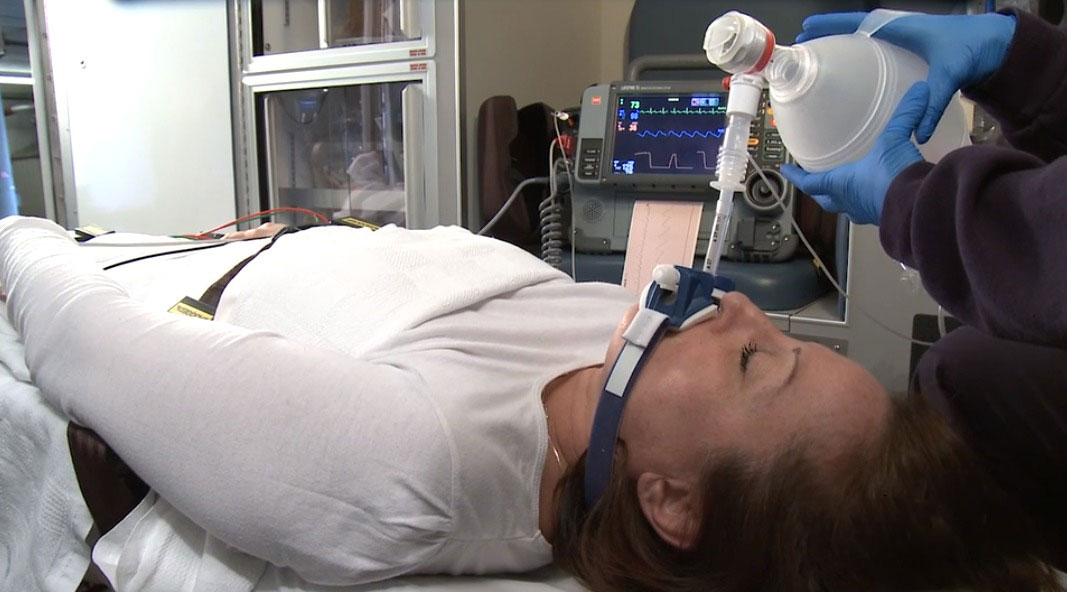
Number two is respiratory failure. When a patient is in respiratory failure, first of all, it's going to be either a hypoxic failure, which is the failure to oxygenate, or hypercapnic failure, which is the failure to ventilate. Either one of these problems can be solved without intubation, but sometimes we end up going that route anyway because we weren't able to fix their problem by other means.
And our third indication is anticipated clinical course of the patient. This indication perhaps requires a little more judgment from the clinician than the other two. What anticipated clinical course means is, do we think we'll need to manage this airway using an advanced method, either in transport or emergently once the patient is at the receiving facility? So some examples of this may be airway burns or inhalation injuries that the airway is doing okay now, the patient may be breathing fine, their airway may be patent, but en route, there is a serious risk of swelling or deterioration: the rapidly deteriorating patient who may not make it to the hospital without being emergently intubated.
So rather than emergently intubate these patients, it's better to have a plan and to be proactive in managing their airway before it becomes an emergency. Again, while skill and technique are very important in airway management, the why and the when are equally as important. And while the actual psychomotor portion of airway management is important, we have to remember that education and assessment are key components of finding out the why and the when. Remember, although this advice is evidence-based and backed by current best practices, always follow your local protocols and guidelines.
When it comes to acute patient care, every minute counts. It's not just about the skills you bring to the scene but the tools you have, too—from a good set of trauma shears to the communication tech that unites you to your colleagues and the hospital care team. If you could reduce treatment times, simplify workflows, replace the radio report, and enable EMS to be a connected part of every patient case, would you do it? Check out this report on how Colorado Springs, Colorado EMS agencies are doing just that.
Editor's Note: This post was originally published in April of 2017 in collaboration with EMS1 and has been refreshed and updated for accuracy and comprehensiveness.
![]()
Why are leading EMS teams choosing Pulsara? EMS and hospital staff (from rural to urban) can instantly and seamlessly communicate event-based patient information, including one-tap team notifications, image sharing, audio/video calls, ETA alerts, etc. right from the Pulsara app. Learn more here.

National Nurses Week kicks off today with National Nurses Day, an important time to acknowledge and appreciate the people who stand at the center of...

Over the past decade, a growing body of research is establishing a powerful consensus: cross-functional, real-time care team communication is a...

In just a few days, one of the world’s largest mass gatherings is taking place—all while we’re asleep. With millions of bunnies descending on...